Hip bursitis is more common in women than men (18% vs. 7%).1 While it is most often associated with middle-aged females, it can also affect young athletes.
The pain caused by hip bursitis can burden normal daily activities and affect one’s quality of life. That’s why it is important to identify and address the issue to prevent further complications.
Fortunately, biomechanical or ergonomic training, exercises, pain management, and other treatment options are available to help prevent and manage pain caused by hip bursitis. Keep reading to learn more.
What is hip bursitis?
Hip bursitis is an inflammation of the fluid-filled sacs around the hip joint, known as bursae. Bursae are located throughout the body in “high traffic” areas to cushion and lubricate between ligaments, tendons, and bones for reduced friction with daily movement. Unfortunately, too much repetition can lead to swelling and pain.2
Hip bursitis is most common on the lateral side (outside edge) of the hip near the widest part of the hips, known as the greater trochanter. It can also be called trochanteric bursitis when affecting this specific area. Other less common areas include the ischial bursa, which sits directly below the “bones” in our buttocks.
Symptoms of hip bursitis include the following:
- Pain or tenderness in the area around the hip joint
- Difficulty walking, squatting, and climbing stairs
- Swelling or redness in the affected area
- Difficulty sleeping on the affected side
- Limited range of motion in the hip joint3
If you are experiencing these symptoms, it is important to consult with your doctor or physical therapist for a proper diagnosis and treatment plan.
What causes hip bursitis?
People at the highest risk of developing hip bursitis include athletes or manual laborers who engage in strenuous physical activity secondary to repetitive overuse. Women are at a higher risk of developing lateral hip bursitis due to their higher Q-angle (aka wider hips), which affects the mechanics of the knee and hips.
Overall, specific underlying factors that can contribute to hip bursitis include the following:
- Age – Bursitis is more common in people over 40 years of age.
- Poor posture – This can lead to biomechanical imbalances and tissue compromise.
- Poor muscular strength and control – Once again contributing to biomechanical changes.
- Overtraining or repetitive motion that gradually wears down local tissues.
- Trauma – Such as a fall or sports-related impact.
- Tension in the lateral leg due to issues like tightness of the iliotibial band (ITB) or hip flexors.
- Overuse of specific muscles that lead to hip imbalances – For example, the tensor fascia lata (TFL), a hip flexor muscle, is meant to be an accessory muscle that aids other larger hip flexor muscles. However, its connection to the ITB can cause problems if it’s overused with daily movements.
Top 5 exercises for hip bursitis
Where you can start on this list of exercises depends on the severity of your pain and what you can tolerate without causing additional aggravation. These exercises will start with the least intense and progress from there. As always, never force anything that hurts, and talk to your physical therapist for more personalized recommendations.
-
ITB standing stretch
A feel-good stretch for the hip and thigh is a great first step in managing hip bursitis pain. Targeting the often problematic ITB is a perfect place to begin.
- Stand comfortably and cross the leg you want to stretch in front of the other.
- Reach the arm on the same side as your front leg up and overhead, gently leaning sideways toward the opposite side.
- Continue leaning until a stretch is felt along the side of the thigh, trunk, and arm.
- Hold for 60 or more seconds, then switch legs. Repeat 2 to 3 times on each side.
For a visual demonstration of this stretch, watch this short video.
-
Hip flexor stretch (kneeling runner’s lunge)

A runner’s lunge targets the hip flexors, which often tighten with hip bursitis.
- Start by kneeling on one knee with the other foot planted firmly in front of you. The leg with the knee touching the ground is the hip you will target.
- Gradually shift your weight and hips forward while keeping the upper body upright, feeling a stretch in the front of your hip and thigh, and the hip extends.
- Hold for 60 or more seconds, then switch sides. Repeat 2 to 3 times on each side.
Other stretches you can add for a well-rounded lower body program include a hamstring stretch, calf stretch, figure-four glute stretch, and quad stretch.
-
Seated hip isometrics
Moving the hips through their full range of motion can feel impossible initially due to hip pain. Isometric exercises that involve tightening the muscles in pain-free “static” positions can help keep the muscles active without aggravating irritated tissues.4 Two primary exercises can be done for the hips.
- Seated band pushouts: While seated, place a circular resistance band (or tie a knot in a normal band) and place it around the thighs just above the knees. Start with a light resistance band and build from there. Gently hold the knees apart from each other at a distance that is comfortable for 10 to 30 seconds. Repeat 2 to 3 times and alternate with the exercise below.
- Seated ball squeezes: Place a pillow or small ball between the knees. Gently squeeze and hold for 5 to 10 seconds for 10 repetitions. Repeat for 2 to 3 sets while alternating with the exercise above.
-
Core and glute work
When dealing with hip dysfunction, activating the muscles of the abdominals and hips in a coordinated fashion is vital. The following 4 exercises offer a well-rounded strength program for the core. Repeat each one for 10 repetitions for 2 to 3 sets.
- Supine march: Lie on your back with your knees bent and feet flat on the floor. Tighten the lower abs (while still breathing and keeping the upper body relaxed), then alternate lifting one foot off the ground while continually keeping the abs tight to prevent rocking of the hips.
- Bridges: Continue lying on your back with your knees and feet flat on the floor at a hip-width distance apart. Keeping the abs tight, now squeeze the butt and lift the lower back off the floor. Lift comfortably as high as possible and hold for 5 to 10 seconds.
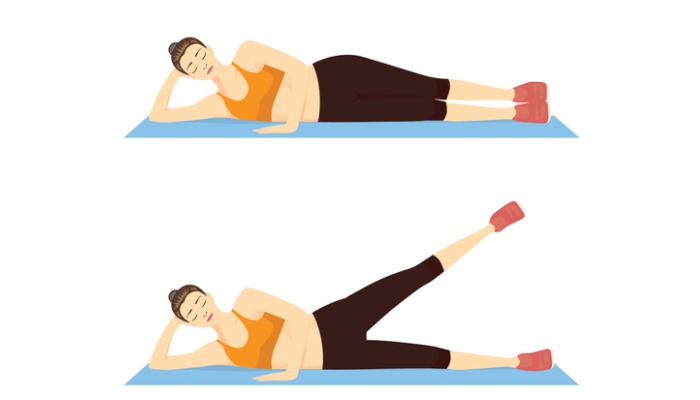
- Clamshells: Lie on your side with your knees bent and stacked on top of each other. Gently lift the top knee away from the bottom one while keeping your feet together. Lift as high as possible without pain or letting the hips roll back. Lower the leg back down with control and repeat.
- Side-lying leg lifts (above image): Stay lying on your side as you did for clamshells, but extend the upper leg straight out in line with the body. Then, lift the leg toward the ceiling while keeping the hip neutral (not flexed or rotated). Once again, keep the hips stacked on top of each other without rolling.
-
Functional strength
In the last stage of recovery, building endurance in the hips that carry over to daily activities is important. Missing this last stage can make it difficult to transition back to normal life.
- Squats: Stand with your feet hip-width apart and facing forward. Start by squatting as low as you can, just to the point that you start feeling too much strain. Then return to standing, tightening the butt muscles and keeping the abdominals firm while maintaining equal weight in both feet.
- Single leg stance: Stand beside a chair or other supportive object for balance. Lift one foot off the ground and hold the position for 30 seconds, then switch legs. Focus on keeping the hips level throughout (not letting one side dip lower). Repeat 2 to 3 times on each side.
- Lunges: Stand in a split stance with one foot forward (knee bent) and the other back (knee straight). Gradually lower yourself into a lunge position by bending the front knee. Then, push through your front heel to return to standing. Repeat on each side for 10 repetitions.
- Resistance band walks: Stand with a resistance band looped around the ankles (or above the knees). Take small steps with the knees slightly bent while keeping tension in the band. Walk sideways for 10 to 15 steps, then switch directions and repeat. Perform this exercise 2 to 3 times on each side. You can also try getting in a deeper squat or walking forward and backward.
Other treatments for hip bursitis
In addition to exercise, one or more of the following treatment options can help expedite the recovery process.
- For short-term pain relief: Talk to your general or orthopedic doctor about anti-inflammatory medications and injections. Natural options such as supplements and essential oils for inflammation may also help. More invasive treatment, such as surgery, is not typically necessary for this health condition.
- Gentle modalities: Pain-relieving holistic options can provide much-needed relief, including electrical stimulation, ultrasound, heat, cold, massage therapy, chiropractic, and acupuncture.
- Work with a physical therapist: They will provide extensive empowering education, a personalized exercise routine, taping, bracing, dry needling/cupping, pain management techniques (including modalities like US), biomechanical training, and much more.5
Professional guidance can keep you on track
While you can do most of your exercises and treatment at home for hip bursitis, professional help can help you feel more confident and ensure that you’re using proper form.
Even with professional guidance, listening to your body’s pain signals and modifying exercises accordingly is important. Keep up with your routine consistently for optimal results. With dedication and patience, you can overcome hip bursitis and get back to living a healthy, active life.
 About JayDee Vykoukal
About JayDee Vykoukal
JayDee Vykoukal is a writer, blogger, Doctor of Physical Therapy, travel enthusiast, and mom of two girls. She is passionate about helping others live their best life via a healthy lifestyle.
Sources:
1. Seidman, A.J., M. Taqi, & M. Varacallo. Trochanteric Bursitis In: StatPearls [Internet] (Treasure Island, FL: StatPearls Publishing, 2023).
2. Planka, M.A., J. Serino, et al. “Greater trochanteric pain syndrome: Evaluation and management of a wide spectrum of pathology.” SAGE Open Medicine (2021): 9.
3. “Trochanteric Bursitis.” Physiopedia. Physio-pedia.com.
4. Clifford, C., L. Paul, et al. “Isometric versus isotonic exercise for greater trochanteric pain syndrome: a randomised controlled pilot study.” BMJ Open Sport & Exercise Medicine 5, no. 1 (2019).
5. Reid, D. “The management of greater trochanteric pain syndrome: A systematic literature review.” Journal of Orthopaedics 13, no. 1 (2016): 15-28.